📅 Published on September 26, 2025 | 🕒 Last updated on March 4, 2026
Lower back pain is one of the most common medical problems in the United States.[1] Emerging evidence indicates that women may experience distinct patterns of lower back pain relative to men—particularly those related to the menstrual cycle, hormonal fluctuations, pregnancy, and gynecological conditions.[2] Certain causes of lower back pain are unique to individuals with the capacity for menstruation, including factors related to pregnancy, endometriosis, menstrual disorders, and other reproductive health conditions.[1][2] Understanding these causes can help patients and clinicians recognize the source of discomfort and select appropriate treatment strategies.
Lower Back Pain in Women
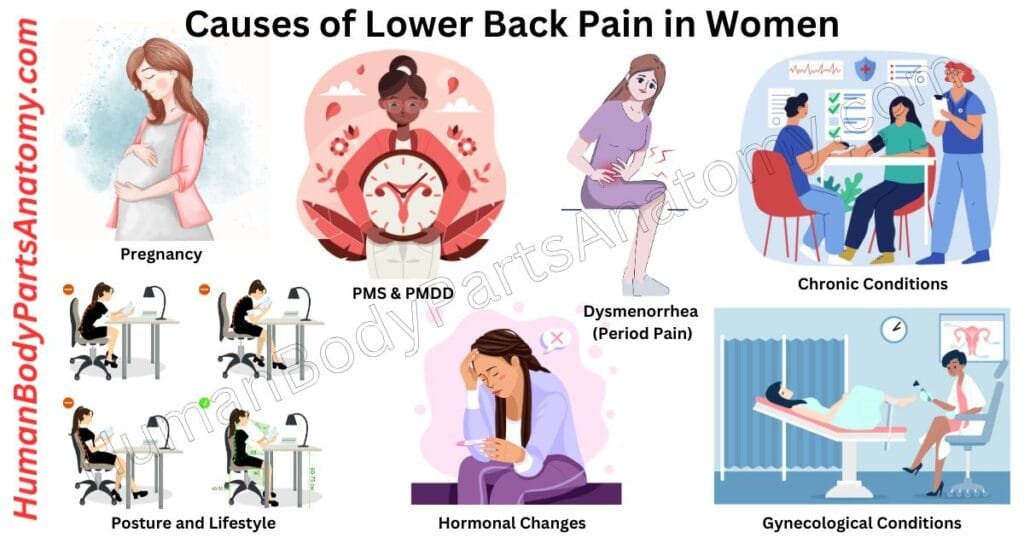
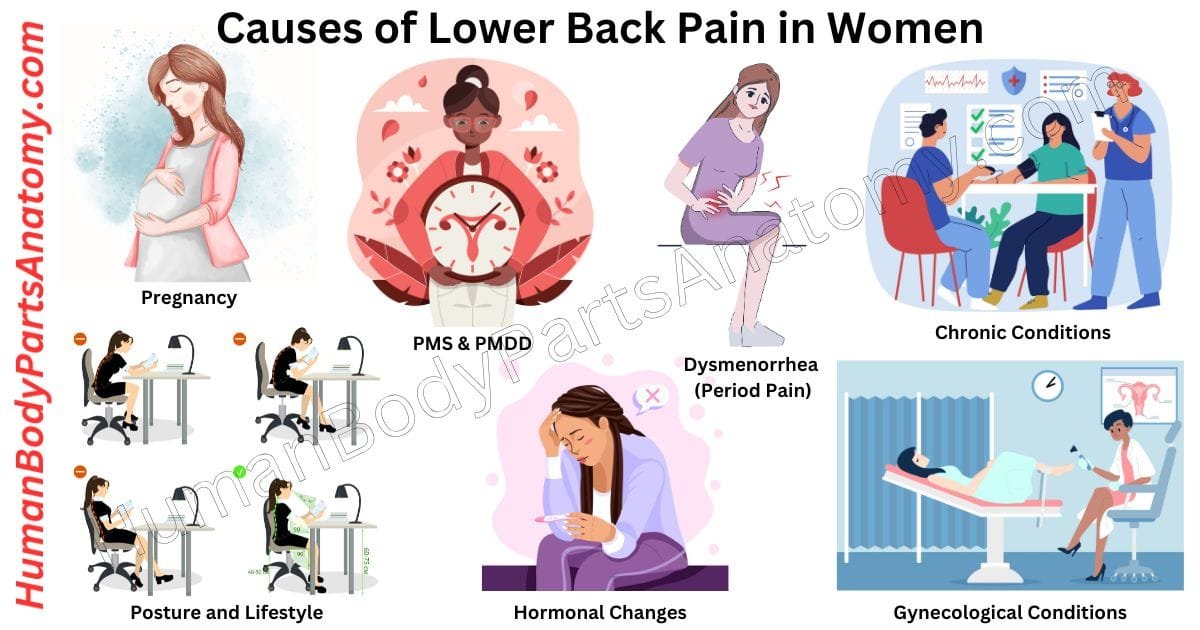
Causes of Low Back Pain in Women
- Hormonal Changes
- Pregnancy
- Gynecological Conditions
- Chronic Conditions
- Dysmenorrhea (Period Pain)
- Premenstrual Syndrome (PMS)
- Premenstrual Dysphoric Disorder (PMDD)
- Posture and Lifestyle
Causes of Lower Back Pain in Women
1. Hormonal Changes
Hormonal changes can have a direct effect on back health, particularly in postmenopausal women. As women age and approach or pass menopause, declining estrogen levels can weaken bones.[2]
Low estrogen is a central factor in the development of osteoporosis—a bone disease in which bone mineral density and bone mass decrease, leading to a reduction in bone strength and an increased risk of fractures.[3]
According to the National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS), osteoporosis is the major cause of fractures in postmenopausal women, with the spine, hip, and wrist being the most commonly affected sites.[3]
When osteoporosis affects the spine, it can cause vertebral compression fractures—where vertebrae gradually collapse under mechanical pressure—often leading to persistent back pain, height loss, and a stooped posture (kyphosis). These sequelae predominantly affect postmenopausal women, though they can occur in men as well.[3]
Additionally, estrogen receptors have been identified within intervertebral disc (IVD) tissue and nearby spinal joints. Research published in Bone Research found that changes in estrogen are an important contributor to both low back pain and osteoarthritis.[4]
These conditions occur more frequently in elderly women than in other populations—and that this disparity is amplified during menopause.[4]
Beyond menopause, progesterone and the pregnancy-related hormone relaxin also influence spinal stability. Elevated progesterone can increase fluid retention and cause swelling in tissues surrounding the spine. During pregnancy, relaxin increases pelvic ligament laxity, which can produce instability in the lower back.[5]
What You Can Do to Protect Your Bones and Back:
- Get adequate calcium and vitamin D: These nutrients are essential for bone health. Dietary sources include dairy products, leafy greens, nuts, and fortified foods. Consult your doctor regarding supplementation needs.[6]
- Schedule regular bone density scans (DEXA scans): According to NIAMS, all women over age 65 should have a bone density test, as osteoporosis is frequently a silent disease with no symptoms until a fracture occurs.[6]
- Engage in weight-bearing exercises: Walking, resistance training, and yoga help strengthen bones and muscles and have been recommended by NIH consensus panels for osteoporosis prevention.[6]
- Avoid smoking and limit alcohol consumption: Both accelerate bone loss and increase fracture risk.[6]
- Discuss hormone health with your doctor: In some cases, hormone therapy may be considered, though benefits must be carefully weighed against potential risks on an individualized basis.[6]
By understanding the link between hormones, bone health, and back pain, you can take preventive measures to stay active, mobile, and pain-free as you age.
2. Pregnancy
Back pain is one of the most common complaints during pregnancy. Research estimates that 95% of pregnant women experience some form of back pain at some point during their pregnancy or in the postpartum period.[5]
According to the American College of Obstetricians and Gynecologists (ACOG), as the baby grows, the expanding uterus shifts the body’s center of gravity and stretches and weakens the abdominal muscles that normally support the spine.[7]
These biomechanical changes—combined with pregnancy-related weight gain and postural adjustments—often lead to lower back pain, particularly in the second and third trimesters.[7]
The pain can range from a dull ache to sharp discomfort, making it harder to sit, stand, or sleep comfortably. Hormonal contributions are also significant: the hormone relaxin, produced during pregnancy, increases pelvic ligament laxity—and research has correlated back pain with elevated relaxin levels.[5][7]
Normal weight gain of 20–40 pounds during pregnancy shifts the center of gravity anteriorly, increasing mechanical stress on the lumbar spine.[5]
How to Relieve Back Pain During Pregnancy
- Wear Supportive Gear: Maternity support belts or belly bands can help distribute your baby’s weight more evenly, reducing strain on your back and hips.[7]
- Practice Pregnancy-Safe Exercises: Gentle stretching, prenatal yoga, and low-impact exercises like walking or swimming can strengthen your core and improve flexibility. Always consult your doctor before starting or modifying any exercise routine.[7]
- Maintain Good Posture: Standing tall with your shoulders back and avoiding slouching can ease pressure on your lower back. When sitting, choose chairs with good lumbar support.[7]
- Sleep Smart: Sleeping on your side with a pillow between your knees or under your belly can provide extra support and reduce back pain.[8]
- Apply Heat or Cold Packs: Using a warm compress or ice pack on sore areas may help relieve discomfort.[8]
By combining these simple lifestyle adjustments with regular prenatal care, most women find relief and enjoy a more comfortable pregnancy.[7]
3. Gynecological Conditions
Certain gynecological conditions are well-established causes of lower back pain in women, with endometriosis and uterine fibroids among the most prevalent.
Endometriosis is a disease in which tissue similar to the lining of the uterus (the endometrium) grows outside the uterus. According to the Eunice Kennedy Shriver National Institute of Child Health and Human Development (NICHD), endometriosis is one of the most common gynecological diseases, affecting an estimated 10% of reproductive-age women—though many go undiagnosed, making this an underestimate.[9]
Its primary symptoms include pain and infertility. Symptoms can include not only pelvic pain but also pain in the lower back or thighs, pain during or after sex, pain during urination or bowel movements, and chronic pelvic pain.[9]
The pain from endometriosis occurs because patches of endometrial-like tissue outside the uterus respond to hormonal cycles in a manner similar to the uterine lining—bleeding and becoming inflamed each menstrual cycle.[9]
The resulting inflammation and chemical mediators can irritate surrounding tissue and nerve endings, producing pain that may radiate to the lower back.[9]
Uterine fibroids (leiomyomas) are non-cancerous growths in or on the muscle of the uterus. They can cause back pain, particularly when they become large or exert pressure on nearby nerves or pelvic structures.[9]
What You Can Do:
- Schedule regular gynecological check-ups: Routine exams help detect problems early before they worsen.[9]
- Understand your treatment options: Depending on the condition, treatment may involve medications, hormone therapy, or surgical procedures. Discuss all options with your gynecologist to find the best approach for your situation.[9]
- Monitor symptoms: Keep track of your pain, menstrual changes, or other unusual symptoms, as this information can help your doctor tailor your treatment.[9]
4. Chronic Conditions
Chronic lower back pain is frequently associated with long-term structural or inflammatory health conditions including osteoarthritis, herniated intervertebral discs, scoliosis, sciatica, spinal stenosis, sacroiliac joint dysfunction, and hip problems.[1]
According to NIAMS, back pain can range from local pain in a specific spot to generalized pain spreading across the back, and may radiate to the buttocks, legs, or abdomen.[1]
Osteoarthritis leads to inflammation and breakdown of cartilage in spinal facet joints, while herniated discs or spinal stenosis may compress spinal nerves, triggering pain, numbness, or tingling. Over time, these conditions can significantly impair daily activities if left untreated.[1]
Women are disproportionately affected by certain chronic conditions. Research published in Bone Research (2023) found that osteoarthritis affects up to twice as many women as men, and this disparity is amplified during menopause—likely due to the protective role of estrogen on joint and intervertebral disc health.[4]
How to Manage Chronic Back Pain
A personalized treatment plan often works best. Common approaches include:
- Physical Therapy – Targeted exercises can strengthen core and back muscles, improve posture, and reduce stress on painful areas. Consistency is key to long-term relief.[1]
- Medications – Over-the-counter pain relievers or prescribed anti-inflammatory drugs may help manage flare-ups. Always follow a doctor’s guidance.[1]
- Injections & Advanced Treatments – Steroid injections, nerve blocks, or radiofrequency ablation may be recommended for severe or persistent pain after thorough evaluation.[1]
- Lifestyle Changes – Maintaining a healthy weight, practicing good posture, and engaging in low-impact activities like swimming or walking can reduce strain on the spine.[1]
- Alternative Therapies – Some people find relief with acupuncture, chiropractic adjustments, or yoga, though results can vary.[1]
5. Dysmenorrhea (Period Pain)
Dysmenorrhea, or painful menstruation, refers to cramping and pain that occur before or during menstrual periods. According to the MedlinePlus Medical Encyclopedia (NIH), the most common form—primary dysmenorrhea—results from an excess of prostaglandins produced in the uterine lining.[10] These chemicals cause uterine muscles and blood vessels to contract, producing cramping and pain.[11]
According to a clinical review in NIH’s StatPearls (2023), dysmenorrhea is one of the most common gynecological problems among all menstruating individuals.[12]
Prevalence estimates range from 16% to 91% in reproductive-age individuals, with severe pain occurring in 2–29% of those affected—and in adolescents, prevalence has been reported as high as 80%.[12]
Painful menstruation is a leading cause of lost time from school and work among women in their teens and twenties.[10]
According to Johns Hopkins Medicine, symptoms may include cramping in the lower abdomen, low back pain, pain spreading to the legs or thighs, nausea, vomiting, diarrhea, fatigue, and headaches.[13]
Secondary dysmenorrhea—caused by conditions such as endometriosis or uterine fibroids—tends to begin later in life, often worsens over time, and may begin days before menstruation and persist after it ends.[11]
Relief and Management Options
- Apply a heating pad, take a warm bath, or use a hot water bottle to relax muscles and reduce cramps.
- Gentle movement: Engaging in light exercise, such as walking, swimming, or yoga, can help improve blood flow and alleviate discomfort.[14]
- Massage the abdomen or lower back gently, and try breathing exercises to reduce tension and pain.[14]
- Over-the-counter medication: Nonsteroidal anti-inflammatory drugs (NSAIDs) like ibuprofen can be effective for pain relief.[10]
- Lifestyle support: Staying hydrated, eating a balanced diet rich in fruits and vegetables, and reducing consumption of caffeine and salty foods may help alleviate bloating and discomfort.[10]
6. Premenstrual Syndrome (PMS)
Premenstrual syndrome (PMS) refers to a constellation of physical, emotional, and behavioral symptoms that commonly occur in the days before menstruation.[15]
According to MedlinePlus (NIH), PMS symptoms typically appear about 5 to 11 days before menstruation and often ease once bleeding begins or within one to two days after.[15]
Symptoms vary widely but can include lower back pain, bloating, headaches, fatigue, mood changes, and irritability.[15]
The exact cause of PMS is not fully established; however, changes in hormone levels during the menstrual cycle are thought to play a significant role—and these hormonal fluctuations may affect some women more than others.[15]
For many women, PMS can be managed effectively through lifestyle modifications including regular aerobic exercise, a balanced diet, reduced caffeine and sodium intake, adequate sleep, and stress management.[15]
When symptoms are more severe, a physician may recommend hormonal birth control, antidepressants (SSRIs), diuretics, or anti-anxiety medications.[15]
7. Premenstrual Dysphoric Disorder (PMDD)
Premenstrual Dysphoric Disorder (PMDD) is a severe form of PMS. The MedlinePlus Medical Encyclopedia (NIH) defines PMDD as a condition in which a woman has severe depression, irritability, and tension before menstruation—with symptoms that are more severe and debilitating than those of typical PMS.[16]
Research at the National Institute of Mental Health (NIMH) has demonstrated that women with PMDD have an abnormal biological sensitivity to normal hormonal changes—even when their hormone levels themselves are within the normal range.[17]
NIMH confirmed this by showing that experimentally suppressing estrogen and progesterone eliminated PMDD symptoms, while reintroducing these hormones triggered their return.[17]
A subsequent NIMH-supported study identified molecular mechanisms underlying this sensitivity, finding that expression of the ESC/E(Z) gene complex—an effector of ovarian steroid response—was systematically disrupted in cells from women with PMDD.[17]
According to the NIMH, PMDD affects approximately 2–5% of women of reproductive age, whereas less severe PMS is considerably more common.[17]
Symptoms—which include mood swings, irritability, fatigue, bloating, headaches, low back pain, and depression—typically appear about one week before menstruation and usually ease within a few days after it begins. A family history of depression, anxiety, or mood disorders may increase susceptibility.[16]
Although PMDD can feel overwhelming, it is treatable. A healthy lifestyle (regular exercise, balanced nutrition, stress management, adequate sleep) can mitigate symptoms. [16][17]
Medically, SSRIs are typically the first-line pharmacological option; certain hormonal contraceptives may also help.[16]
8. Posture and Lifestyle
Many instances of lower back pain are linked to modifiable daily habits rather than underlying structural pathology.[1]
According to NIAMS, risk factors include sedentary behavior, poor physical fitness, excess body weight, and occupational exposures such as heavy lifting or prolonged sitting.[1]
When the core muscles that support the spine are weak—due to inactivity or other factors—the spine is subjected to greater mechanical stress.[1]
NIAMS notes that back pain is more common among people who are not physically fit and that weak back and abdominal muscles may not adequately support the spine.[1]
Practical Tips to Protect Your Back:
- Check your posture regularly: Adjust your chair, desk, and computer screen so you sit upright with both feet flat on the floor. Use a chair that supports your lower back.[1]
- Move often: Take short breaks to stretch or walk if you sit for long periods. Even a few minutes of movement every hour helps reduce stiffness.[1]
- Lift safely: Always bend at your knees and keep the object close to your body instead of bending at your waist.[1]
- Strengthen your core: Simple exercises like planks, bridges, or gentle yoga can improve stability and protect your spine.[1]
- Stay active: Regular walking, swimming, or cycling improves circulation and keeps your back muscles strong.[1]
FAQ’s-
Some cancers in women can cause lower back pain, especially if they press on nerves, bones, or organs in the pelvic or abdominal area. These include:
Ovarian cancer – may cause pelvic or lower back pain, bloating, and abdominal fullness.
Uterine (endometrial) cancer – can cause back pain along with abnormal vaginal bleeding.
Cervical cancer – may lead to lower back pain if it spreads, often with pelvic discomfort or unusual bleeding.
Kidney or bladder cancer – tumors can press on the lower back, sometimes causing blood in urine.
Metastatic cancers – cancers from the breast, lung, or other organs can spread to the spine or pelvis, causing persistent back pain.
In women, common causes include muscle or ligament strain, hormonal changes during the menstrual cycle or menopause,[2] gynecological conditions such as endometriosis or uterine fibroids,[9] pregnancy-related postural and biomechanical changes,[7] age-related spinal degeneration, herniated discs, sacroiliac joint dysfunction, and pelvic inflammatory disease.[1]
Some women notice more lower back pain during their menstrual cycle, perimenopause, or times of hormonal changes. This can happen due to shifts in pelvic muscles, inflammation, or pain that radiates from the uterus or ovaries.[2]
Research shows that women are slightly more likely to experience lower back pain, often due to pregnancy, hormonal changes, or gynecological and obstetric conditions.[2][4]
Conservative therapies are often the first-line approach and include physical therapy, targeted exercises and stretching, heat or ice therapy, over-the-counter NSAIDs, postural correction, and core muscle strengthening.[1] For condition-specific causes, additional treatments—such as hormonal therapy for menstrual disorders or endometriosis, or surgical intervention for fibroids—may be necessary, as determined by individualized clinical assessment.[9]
Back pain is very common during pregnancy, often beginning in the second or third trimester, though some women report onset as early as weeks 8–12.[5] It typically results from weight gain, anterior shift in the center of gravity, loosening of pelvic ligaments from pregnancy hormones (especially relaxin), and postural changes.[5] According to ACOG, for most women the discomfort improves after childbirth, but back pain may linger for months after delivery in some cases.[7]
References-
- National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS), National Institutes of Health (NIH). Back Pain: Causes, Symptoms, and Treatments. Bethesda (MD): U.S. Department of Health and Human Services; 2023. Available from: https://www.niams.nih.gov/health-topics/back-pain
- Stieger A, et al. Women’s Pain Management Across the Lifespan—A Narrative Review of Hormonal, Physiological, and Psychosocial Perspectives. Journal of Clinical Medicine. 2025; PMCID: PMC12112123. Available from: https://pmc.ncbi.nlm.nih.gov/articles/PMC12112123/
- National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS), National Institutes of Health (NIH). Osteoporosis: Overview, Causes, and Risk Factors. Bethesda (MD): U.S. Department of Health and Human Services; 2022. Available from: https://www.niams.nih.gov/health-topics/osteoporosis
- Pang H, et al. Low back pain and osteoarthritis pain: a perspective of estrogen. Bone Research. 2023; Nature Portfolio. doi:10.1038/s41413-023-00280-x. Available from: https://www.nature.com/articles/s41413-023-00280-x
- Salari N, Mohammadi A, Hemmati M, et al. The global prevalence of low back pain in pregnancy: a comprehensive systematic review and meta-analysis. BMC Pregnancy and Childbirth. 2023 Dec 2;23(1):830. doi:10.1186/s12884-023-06151-x. PMID: 38042815. Available from: https://pubmed.ncbi.nlm.nih.gov/38042815/
- National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS), National Institutes of Health (NIH). Osteoporosis: Diagnosis, Treatment, and Steps to Take. Bethesda (MD): U.S. Department of Health and Human Services; Last reviewed December 2022. Available from: https://www.niams.nih.gov/health-topics/osteoporosis/diagnosis-treatment-and-steps-to-take
- American College of Obstetricians and Gynecologists (ACOG). Back Pain During Pregnancy (Patient FAQ). Washington (DC): ACOG; 2021. Available from: https://www.acog.org/womens-health/faqs/back-pain-during-pregnancy
- Cleveland Clinic. Back Pain During Pregnancy: Causes and Relief. Cleveland (OH): Cleveland Clinic Foundation; 2024. Available from: https://my.clevelandclinic.org/health/symptoms/back-pain-during-pregnancy
- World Health Organization (WHO). Endometriosis. Fact Sheet. Geneva: WHO; Updated 15 October 2025. Available from: https://www.who.int/news-room/fact-sheets/detail/endometriosis
- MedlinePlus Medical Encyclopedia, National Library of Medicine (NLM), National Institutes of Health (NIH). Painful Menstrual Periods (Dysmenorrhea). Bethesda (MD): U.S. National Library of Medicine; 2024. Available from: https://medlineplus.gov/ency/article/003150.htm
- American College of Obstetricians and Gynecologists (ACOG). Dysmenorrhea: Painful Periods (Patient FAQ). Washington (DC): ACOG; 2022. Available from: https://www.acog.org/womens-health/faqs/dysmenorrhea-painful-periods
- Nagy H, Khan MAB. Dysmenorrhea. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023. NCBI Bookshelf ID: NBK560834. Available from: https://www.ncbi.nlm.nih.gov/books/NBK560834/
- Johns Hopkins Medicine. Dysmenorrhea: Symptoms, Causes, and Treatments. Baltimore (MD): Johns Hopkins University School of Medicine; 2024. Available from: https://www.hopkinsmedicine.org/health/conditions-and-diseases/dysmenorrhea
- Mayo Clinic. Menstrual Cramps: Diagnosis and Treatment. Rochester (MN): Mayo Foundation for Medical Education and Research; 2022. Available from: https://www.mayoclinic.org/diseases-conditions/menstrual-cramps/diagnosis-treatment/drc-20374944
- MedlinePlus, National Library of Medicine (NLM), National Institutes of Health (NIH). Premenstrual Syndrome (PMS). Bethesda (MD): U.S. National Library of Medicine; 2024. Available from: https://medlineplus.gov/premenstrualsyndrome.html
- MedlinePlus Medical Encyclopedia, National Library of Medicine (NLM), National Institutes of Health (NIH). Premenstrual Dysphoric Disorder (PMDD). Bethesda (MD): U.S. National Library of Medicine; 2024. Available from: https://medlineplus.gov/ency/article/007193.htm
- National Institute of Mental Health (NIMH), National Institutes of Health (NIH). Sex Hormone–Sensitive Gene Complex Linked to Premenstrual Mood Disorder. Bethesda (MD): U.S. Department of Health and Human Services; 2017. Available from: https://www.nimh.nih.gov/news/science-updates/2017/sex-hormone-sensitive-gene-complex-linked-to-premenstrual-mood-disorder
Medical Disclaimer
All content on HumanBodyPartsAnatomy.com is educational and based on verified, peer-reviewed medical sources. Articles are authored or reviewed by qualified medical or biomedical professionals to ensure accuracy.
This website does not provide medical advice, diagnosis, or treatment. Always consult a licensed healthcare professional for personal medical guidance.
No commercial or promotional interests influence the medical content published on this site.