📅 Published on September 24, 2025 | 🕒 Last updated on March 27, 2026
- Lower back pain (LBP) is one of the leading causes of disability worldwide, affecting up to 80% of adults at some point in their lives.
- The most common causes include muscle overuse, intervertebral disc injury, degenerative disc disease, spondylolisthesis, spinal stenosis, scoliosis, and compression fractures.
- LBP is classified as acute (<6 weeks), sub-acute (6–12 weeks), or chronic (>12 weeks).
- Most acute episodes resolve with conservative management; chronic cases require a multidisciplinary approach.
- Red flag symptoms—such as progressive leg weakness, bladder/bowel dysfunction, or unexplained weight loss—warrant urgent medical evaluation.
- Preventive strategies, including core strengthening, weight management, and ergonomic corrections, can significantly reduce recurrence.
Overview of Lower Back Pain Causes
Lower back pain (LBP) is one of the most prevalent and costly musculoskeletal conditions in the United States, ranking as a leading cause of missed workdays, disability, and reduced quality of life. According to the Global Burden of Disease study, LBP affects an estimated 619 million people globally, with projections suggesting that number will exceed 843 million by 2050.
The lumbar spine—comprising five vertebrae (L1–L5), intervertebral discs, facet joints, ligaments, and paraspinal musculature—is an intricate, load-bearing structure that supports nearly every movement the body makes. Its complexity makes it vulnerable to a wide range of mechanical, degenerative, and pathological insults.
While the onset of LBP often follows a specific physical trigger—such as lifting, twisting, or prolonged sitting—the underlying etiology is frequently multifactorial, involving structural, biomechanical, and psychosocial components. Understanding the precise cause is essential for selecting the most effective treatment strategy.
Clinical Perspective
Age-related spinal degeneration does not inevitably cause debilitating pain. Research shows that many individuals—including athletes in their 70s and 80s—demonstrate significant disc degeneration on MRI yet remain functionally active. Pain experience is shaped by biological, psychological, and social factors.
Let’s study the most common causes of lower back pain, exploring their underlying factors and how they affect overall spinal health.
Key Anatomical Structures Involved in Lower Back Pain
A foundational understanding of lumbar anatomy helps contextualize why and how pain develops:
- Intervertebral Discs: Fibrocartilaginous cushions between vertebrae. Each disc has a tough outer ring (annulus fibrosus) and a gel-like core (nucleus pulposus) that absorbs compressive forces.
- Facet Joints: Paired synovial joints at each spinal level that guide and limit movement. Subject to arthritic degeneration over time.
- Paraspinal Muscles & Ligaments: Provide dynamic stability to the spine. Overuse or acute strain is the single most common source of LBP in active adults.
- Nerve Roots: Exit the spinal canal through neural foramina. Compression or irritation causes radicular pain (sciatica), numbness, or motor weakness.
- Sacroiliac (SI) Joints: Connect the lumbar spine to the pelvis. Dysfunction in these joints can closely mimic lumbar disc pathology.
Causes of Lower Back Pain Diagram
What Causes Lower Back Pain
- Muscle and Ligament Strain (Overuse Injury)
- Intervertebral Disc Injury
- Annular Tear (Disc Tear)
- Herniated Disc (Disc Herniation / Slipped Disc)
- Degenerative Disc Disease (DDD)
- Degenerative Spondylolisthesis
- Spinal Stenosis
- Scoliosis
- Compression Fracture
Lower Back Pain Causes
LBP etiologies are broadly categorized as specific (identifiable structural or systemic pathology) and nonspecific (no definitive structural cause identified). Approximately 85–90% of LBP cases are classified as nonspecific. The following are the most clinically significant causes:
1. Muscle and Ligament Strain (Overuse Injury)
Muscular or ligamentous strain is the most common trigger of acute lower back pain, particularly in younger, active individuals. It occurs when the paraspinal muscles, erector spinae, multifidus, or associated ligaments are stretched beyond their physiological range—resulting in micro-tears, inflammation, and protective spasm.
Common Triggers: Sudden heavy lifting without proper form, unaccustomed physical activity (e.g., first session after prolonged inactivity), prolonged static postures, sports participation, or repetitive axial loading.
The pain is typically dull or aching, worsens with movement, and is localized to the lower lumbar region. Most episodes resolve within 4–6 weeks with activity modification, analgesics, and progressive mobilization.
Practical Tip
Gradual training progression (the 10% rule—increasing activity volume by no more than 10% per week), adequate warm-up, and maintaining core strength significantly reduce the risk of recurrent strain injuries.
2. Intervertebral Disc Injury
The intervertebral discs are among the most commonly injured structures in the lumbar spine, with two principal pathologies:
Annular Tear (Disc Tear)
The annulus fibrosus—the disc’s outer fibrous shell—can develop radial or circumferential fissures due to cumulative mechanical stress, sudden loading, or natural aging.
These tears may be asymptomatic or produce localized, deep, and often chronic lumbar pain, particularly with flexion and axial loading.
Why some patients experience severe pain from annular tears while others remain symptom-free is not fully understood, but inflammatory mediators (such as phospholipase A2 and prostaglandins) released at the tear site are thought to sensitize adjacent nerve fibers—even in the absence of frank nerve compression.
Herniated Disc (Disc Herniation / Slipped Disc)
Disc herniation occurs when the nucleus pulposus protrudes through a weakened or torn annulus fibrosus. Depending on the degree and direction of herniation, this can impinge upon the dural sac, nerve roots, or, less commonly, the spinal cord itself.
Clinical Presentation: Lumbar herniation most commonly affects the L4–L5 and L5–S1 levels, compressing the sciatic nerve and producing classic sciatica—sharp, shooting, or burning pain that radiates from the lower back through the buttock and down the posterior or lateral leg, often accompanied by numbness, tingling (paresthesia), or focal muscle weakness.
Risk Factors: Repetitive flexion-rotation movements, heavy lifting, sedentary lifestyle, obesity, smoking, and prior disc degeneration.
3. Degenerative Disc Disease (DDD)
As we age, the intervertebral disks in our spine naturally start to wear down and lose height. In some cases, these disks may collapse completely, causing the facet joints to rub against each other.
This friction can lead to pain, stiffness, and reduced mobility. Lifestyle factors, such as smoking, can accelerate this disk degeneration and worsen symptoms.
The gradual wear and tear of these facet joints is known as osteoarthritis or spondylosis.
Over time, this condition can contribute to other spine issues. These issues are spinal stenosis, where the spinal canal narrows and places pressure on nerves, potentially causing numbness, tingling, or weakness in the legs.
Preventive strategies can slow spinal degeneration and improve overall back health. These include:
- Maintaining a healthy weight to reduce stress on the spine
- Staying physically active with exercises that strengthen core and back muscles
- Avoiding smoking and limiting activities that strain the back
- Practicing good posture to reduce wear on disks and joints
4. Degenerative Spondylolisthesis
Spondylolisthesis refers to the anterior displacement of one vertebral body relative to the one below it. The degenerative variant—most common in adults over 50, particularly postmenopausal women—results from progressive facet joint arthropathy and ligamentous laxity, which compromise the segmental stability of the lumbar spine.
The L4–L5 segment is most frequently affected. Slippage compresses exiting nerve roots or narrows the central canal, producing back pain, neurogenic claudication (leg pain and fatigue worsened by walking or standing, relieved by sitting or forward flexion), and occasionally bowel or bladder dysfunction in severe cases.
5. Spinal Stenosis
Spinal stenosis is a condition where the spaces inside your spine become narrower, putting pressure on your spinal cord or the nerves that pass through small openings called neural foramina. This pressure can cause symptoms like pain, numbness, or muscle weakness.
Spinal stenosis is more common as people age, but some are born with a spine that has less space for the spinal cord.
Several factors can contribute to this condition, including aging, thickened bones and ligaments, arthritis of the spine, bone diseases, herniated discs, or injuries.
If you’re experiencing back pain or discomfort, spinal stenosis may be a reason, and early diagnosis can help manage the symptoms effectively.
6. Scoliosis
Scoliosis is a condition where the spine curves abnormally, forming an “S” or “C” shape instead of a straight line. It often develops in children and teenagers during growth spurts, but adults—especially those with arthritis—can also develop it.
This spinal condition can lead to back pain and, in some cases, may cause weakness, numbness, or pain in the legs if the nerves are affected.
Early detection is important, as timely treatment can help manage symptoms and prevent the curve from worsening.
7. Compression Fracture
Compression fractures happen when one or more vertebrae become cracked or broken. The most common cause of these fractures is osteoporosis, a condition where bones become weak and brittle. As people age, bones often lose calcium and other important minerals, making them more prone to fractures.
Besides osteoporosis, compression fractures can also result from:
- Injury or trauma to the back
- Cancer that spreads to the bones from other parts of the body
- Cancers that begin in the spine, such as multiple myeloma
When multiple compression fractures occur, it can cause a condition called kyphosis. Kyphosis is a forward curvature of the spine that creates a noticeable hump-like appearance.
Signs & Symptoms of Lower Back Pain
Low back pain (LBP) is a common condition that can range from a dull, persistent ache to sharp, intense pain. In many cases, the pain may spread to other areas, especially the legs, causing additional discomfort.
LBP can limit movement, making daily activities, work, school, and social participation more difficult. It can also affect sleep, mood, and overall well-being.
Types of Low Back Pain
- Acute LBP: Lasts less than 6 weeks and often improves on its own.
- Sub-acute LBP: Persists for 6–12 weeks.
- Chronic LBP: Lasts more than 12 weeks and may require ongoing management.
While most people with acute LBP recover fully, some cases progress to chronic pain, which can significantly impact quality of life.
Common Symptoms
- Pain Quality: Dull and aching (muscular), sharp or stabbing (facet/disc), electric or burning (neuropathic/radicular).
- Pain Onset: Abrupt (strain, fracture) or insidious (degeneration, stenosis, malignancy).
- Radiation Pattern: Localized to the lumbosacral region, or radiating into the buttocks, posterior thigh, calf, or foot (sciatica/radiculopathy).
- Posture Disturbance: Antalgic lean (lateral trunk shift), loss of lumbar lordosis, or difficulty achieving upright stance.
- Stiffness and Reduced ROM: Most pronounced in the morning or after prolonged inactivity; improves with gentle movement.
- Muscle Spasm: Involuntary, painful tightening of paraspinal muscles—a protective response to underlying tissue injury.
Radicular Symptoms (Sciatica)
Sciatic nerve compression—most commonly from disc herniation or foraminal stenosis at L4–L5 or L5–S1—produces a characteristic syndrome of unilateral lower extremity pain, paresthesia, and potentially motor deficit.
True sciatica follows a dermatomal distribution, distinguishing it from referred somatic pain, which tends to be more diffuse and poorly localized.
Impact on Daily Functioning
Chronic LBP extends well beyond physical symptoms. Research consistently demonstrates strong associations between persistent LBP and depression, anxiety, sleep disturbance, cognitive impairment, and reduced social participation.
In occupational settings, chronic LBP is a leading cause of presenteeism, long-term work absence, and premature retirement.
Red Flag Symptoms: When to Seek Immediate Medical Attention
The following symptoms—individually or in combination—may indicate a serious underlying pathology (infection, malignancy, cauda equina syndrome, fracture) and require urgent clinical evaluation:
- Bladder or bowel incontinence or retention (possible cauda equina syndrome—a surgical emergency)
- Progressive bilateral leg weakness or saddle anesthesia (perineal numbness)
- Severe, unrelenting pain not relieved by any position, particularly at night
- Unexplained significant weight loss (>10 lbs in 6 months without intent)
- History of malignancy with new-onset back pain
- Recent significant trauma (motor vehicle accident, fall from height)
- Fever, chills, or recent invasive procedure (raises concern for spinal epidural abscess or discitis)
- Age > 70 with new-onset back pain (increased fracture and malignancy risk)
Risk Factors for Lower Back Pain
Certain biological, behavioral, and environmental factors substantially elevate an individual’s risk of developing LBP or experiencing its recurrence. Understanding these variables supports targeted prevention.
Non-Modifiable Risk Factors
- Age: Incidence and severity of LBP rise progressively from the third decade, peaking around age 40–60. Spinal degeneration accelerates with each passing decade.
- Biological Sex: Women face higher lifetime risk of LBP, particularly in association with pregnancy, osteoporosis, and hormonal changes that affect connective tissue laxity.
- Genetic Predisposition: Heritability studies suggest that 30–60% of disc degeneration risk is genetically determined. Conditions such as scoliosis, spondylolisthesis, and Scheuermann’s kyphosis also demonstrate familial clustering.
- Prior LBP Episodes: A history of LBP is the single strongest predictor of future episodes.
Modifiable Risk Factors
- Physical Inactivity and Deconditioning: Weak core musculature (transversus abdominis, multifidus) reduces spinal stability and increases disc and facet loading. Regular exercise—particularly core-stabilizing and aerobic activities—is among the most evidence-supported preventive strategies.
- Obesity and Excess Body Weight: Adiposity—particularly central/abdominal obesity—increases lumbar compressive forces, accelerates disc degeneration, promotes systemic inflammation, and is independently associated with chronic LBP.
- Occupational Hazards: Heavy manual labor, repetitive lifting and bending, prolonged sedentary work, and whole-body vibration (heavy vehicle operators) are well-established occupational LBP risk factors.
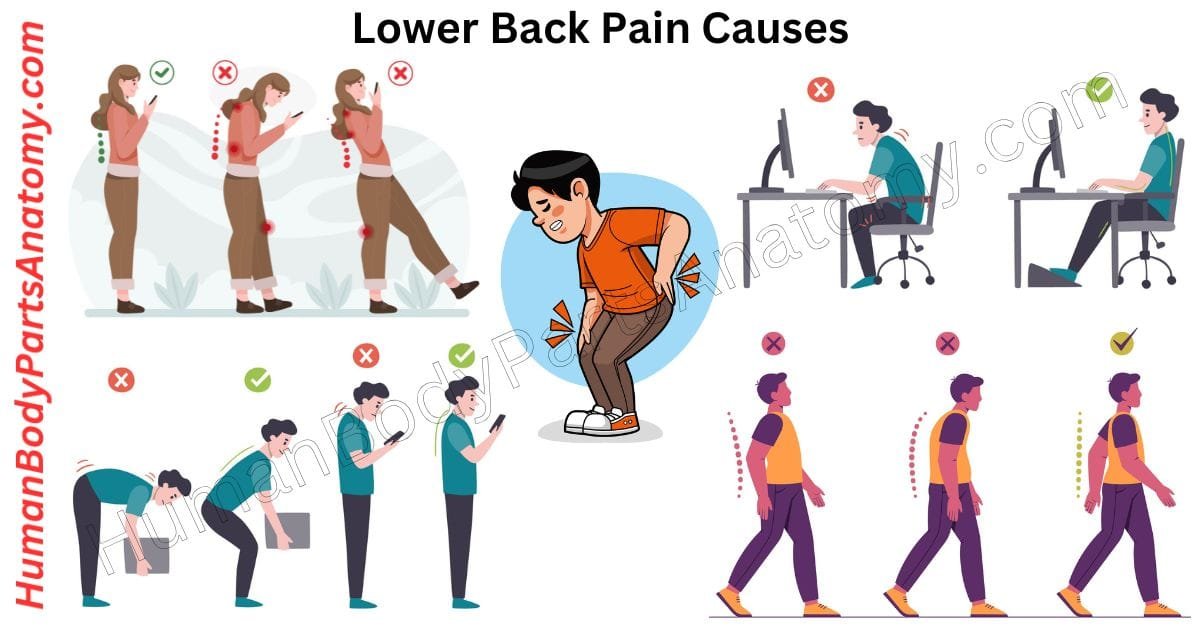
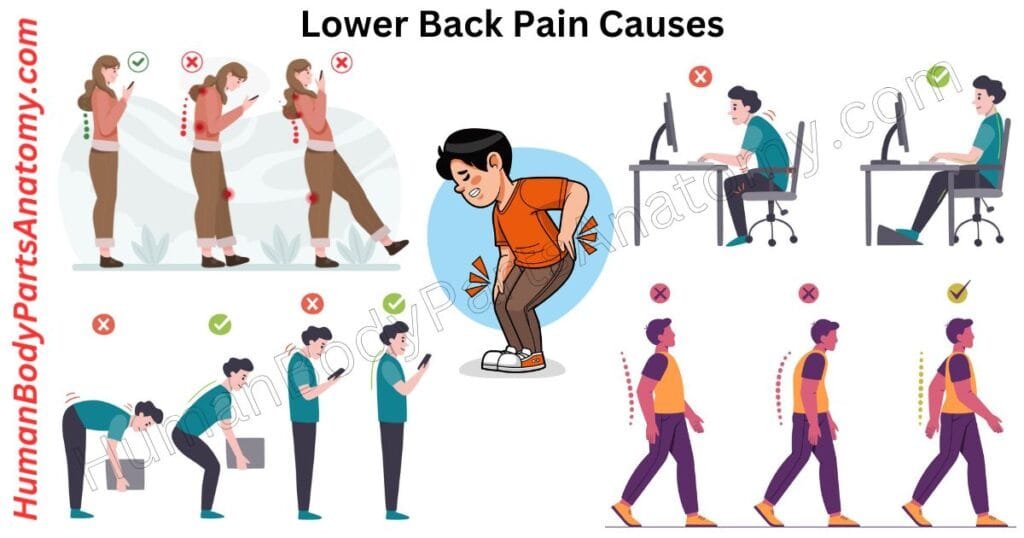
- Poor Ergonomics: Non-ergonomic workstation setup, prolonged sitting without lumbar support, and poor monitor or keyboard positioning contribute to cumulative spinal loading and paraspinal muscle fatigue.
- Cigarette Smoking: Nicotine impairs vertebral endplate vascularity, reducing disc nutrition and accelerating degeneration. Smoking also causes chronic cough, which repeatedly increases intradiscal pressure.
- Psychosocial Factors: Depression, anxiety, catastrophizing, and workplace dissatisfaction are among the strongest predictors of LBP chronification and poor treatment outcomes—often more predictive than structural imaging findings.
- Improper Lifting Mechanics: Lumbar flexion-rotation under load dramatically increases intradiscal pressure and annular stress. Training in neutral-spine lifting technique is a cornerstone of occupational health programs.
Prevention Strategies: Protecting Your Lumbar Spine
Evidence supports the following strategies for reducing the incidence, recurrence, and progression of lower back pain:
- Core Strengthening: Progressive exercises targeting the deep stabilizers (transversus abdominis, lumbar multifidus) and global movers (erector spinae, gluteals) provide essential dynamic support to the lumbar spine.
- Regular Aerobic Exercise: Walking, swimming, cycling, and low-impact aerobics maintain spinal mobility, improve disc nutrition through cyclic loading, and reduce central sensitization.
- Weight Management: Even modest weight reduction (5–10% of body weight) can significantly reduce lumbar compressive forces and inflammatory burden.
- Smoking Cessation: Supported cessation programs reduce both the biological and behavioral contributors to LBP.
- Ergonomic Optimization: Adjustable chairs with lumbar support, monitor positioning at eye level, sit-stand workstations, and regular microbreaks reduce cumulative spinal strain in desk workers.
- Mental Health and Stress Management: Mindfulness-based stress reduction (MBSR), cognitive behavioral therapy (CBT), and adequate sleep have demonstrated efficacy in reducing LBP risk and improving chronic pain outcomes.
Conclusion
Lower back pain is a complex, multidimensional condition that spans a spectrum from self-limiting musculoligamentous strain to progressive neurological compromise.
While the majority of episodes are benign and resolve with conservative care, a thorough understanding of the underlying anatomy, pathophysiology, and clinical presentation is essential for accurate diagnosis, effective treatment, and meaningful prevention.
The field has evolved substantially beyond the traditional biomedical model: psychosocial contributors, lifestyle factors, and central sensitization mechanisms are now recognized as integral to both the onset and persistence of LBP.
Clinicians and patients alike benefit from this holistic understanding—one that moves from merely treating pain episodes to building long-term spinal resilience.
If you or a patient are experiencing persistent or worsening lower back pain, early consultation with a qualified spine specialist, physical therapist, or primary care physician remains the most effective first step toward recovery.
FAQ’s
In the general population, lumbar muscle and ligament strain—typically from overuse, sudden unaccustomed activity, or improper lifting—is the most frequent cause. In clinical settings, disc herniation, degenerative disc disease, and lumbar spondylosis are among the most common structural diagnoses.
Yes. Psychological stress activates the hypothalamic-pituitary-adrenal (HPA) axis, increases cortisol, and triggers sustained paraspinal muscle tension—all of which can cause or perpetuate LBP. The biopsychosocial model of pain recognizes that emotional and cognitive factors are not just “secondary” contributors but primary drivers of pain experience and chronification.
Spinal discs act as cushions between vertebrae. When they wear out or bulge, they can press on nearby nerves, causing pain, tingling, or weakness.
The facet joints, intervertebral joints, and sacroiliac joints are often involved. Degeneration, inflammation, or misalignment in these joints can contribute to discomfort.
Severe or worsening pain, leg numbness, muscle weakness, difficulty walking, or changes in bladder or bowel function are signs that require immediate medical care.
There is a meaningful genetic component to several conditions underlying LBP, including intervertebral disc degeneration, scoliosis, spondylolisthesis, and osteoporosis. Twin studies demonstrate heritability estimates of 30–60% for disc degeneration. Family history is therefore a clinically relevant risk factor.
Yes. Constipation can cause lower back pain when backed-up stool increases pressure on the lower spine and surrounding nerves, leading to discomfort or aching. Pain may improve once bowel movements become regular, but persistent symptoms should be evaluated by a healthcare provider.
Yes. Uterine fibroids—noncancerous growths in the uterus—can cause lower back pain if they grow large enough to press on pelvic nerves or nearby structures. This pain may feel dull, aching, or persistent and is often associated with heavy menstrual bleeding or pelvic pressure.
Lower back pain just above the buttocks is commonly caused by muscle strain, poor posture, sacroiliac (SI) joint dysfunction, or lumbar disc issues. It may also result from overuse, prolonged sitting, or underlying spinal conditions that affect the lower lumbar region.
Lower back pain is most often caused by muscle strain, poor posture, repetitive movements, or age-related spinal changes such as disc degeneration. In some cases, it may signal nerve compression, arthritis, kidney problems, or other medical conditions—especially if pain is severe, persistent, or accompanied by numbness or fever.
Medical Disclaimer
All content on HumanBodyPartsAnatomy.com is educational and based on verified, peer-reviewed medical sources. Articles are authored or reviewed by qualified medical or biomedical professionals to ensure accuracy.
This website does not provide medical advice, diagnosis, or treatment. Always consult a licensed healthcare professional for personal medical guidance.
No commercial or promotional interests influence the medical content published on this site.